The Big Picture
Headlines focusing on burnout, frustration and a mass exodus of nurses have been omnipresent for the better part of two years. Countless surveys have sought to quantify the level of risk facing our healthcare system’s caregivers. And, by extension, the level of risk facing our healthcare system.
If nurses are headed for the exits, an already significant shortage could turn catastrophic. At the same time, nurses who are unhappy but choose to stay can lead to a different set of problems, with a disgruntled workforce creating cracks from within.
The potential disaster is well known, as are some obvious interventions – higher pay and more staffing top the list. But with hospital finances also precarious, alternatives are needed.
To better grasp what those alternatives might be and how healthcare leaders can pursue them, Jarrard Inc. polled nurses across the country. The results offer insight into what these caregivers find valuable, whom they trust, how they feel about their work environment – and how that correlates with feelings about pay – and how communications can help boost the healthcare workforce.
The online survey collected responses from 1,078 RNs, APRNs, RNs and CRNAs working in hospitals, outpatient clinics and health service organizations. It was fielded in September 2022 – a time when the healthcare system was well beyond the COVID-19 crush but still deeply strained, and when nurses in many locations were evaluating their options, organizing and pushing for change.
Indeed, we found that just over one in four nurses are satisfied with their pay. Some positives: Two thirds are satisfied with their job and three quarters are likely to remain in nursing. Yet only a quarter are very satisfied, and similar number are very likely to remain.
Among those who are dissatisfied with their pay, their trust in administration, perception of recognition programs and views on executive rounding are all more negative than among those who feel their pay is appropriate for the work they do.
Can anything else resonate with nurses in the absence of higher pay? Are well-intentioned tactics exacerbating the problem? Does dissatisfaction with pay spill over into other areas?
On distilling this survey, the Jarrard Inc. team has identified opportunities for leaders to help their organizations bolster the nursing workforce when the obvious answer of “higher pay” is off the table. And, it provides encouragement to resist the urge to do something instead of nothing when those things might actually make the problem worse. Our recommendations show how to use the power of communications to make a strategic difference with meaningful ROI.
Key Findings
The Nursing Workforce is Fragile
A minority of nurses feel their pay is appropriate, and only a quarter are very satisfied with their job. On the bright side, 75 percent are at least somewhat likely to stay in the field.
Anything Done Out of Habit is Worth Revisiting
Global gestures and calendar dates like Hospital Week aren’t landing the way leadership teams would like. Changes are needed to get a better ROI from nurse engagement efforts.
Trust is Highest at the Ground Level
Direct managers and nursing colleagues are nurses’ most trusted sources of information. CEOs take last place – even more so among nurses dissatisfied with their pay.
Engagement Tactics are Not One-Size-Fits-All
“Micro-communications” and targeted outreach are needed. For instance, elements like increased PTO and proper staffing levels matter more to older nurses and those who are dissatisfied, while interaction with leadership is more popular among younger nurses and those who feel they’re paid appropriately.
Present, Engaged and Authentic Leadership Can Help
Nurses called out pizza parties and knick-knacks as efforts more likely to harm morale than help. Meanwhile, having managers and administrators who are visible, communicative and responsive can be viewed in a positive light.
The Core Imperative
In discussing these results with our clients across the country, one thing became immediately clear: The findings, while not surprising, are deeply compelling for communications teams. That’s because they give weight to the gut feelings and experiences of communications leaders who are striving each day to engage the nursing workforce. This data allows them to reinforce with executive leadership teams the need to rethink and adapt. We show a clear need and opportunity to revisit old habits. Continuing to run with the same, one-size-fits-all approach to communications, engagement and recognition programs is no longer enough to connect with nurses. Communications teams have a vital role in ensuring this gets the proper prioritization from the C-Suite. From there, communications must be at the center of efforts to listen to nurses and tailor engagement efforts to what will actually resonate.
Finding 1: The nursing workforce is fragile
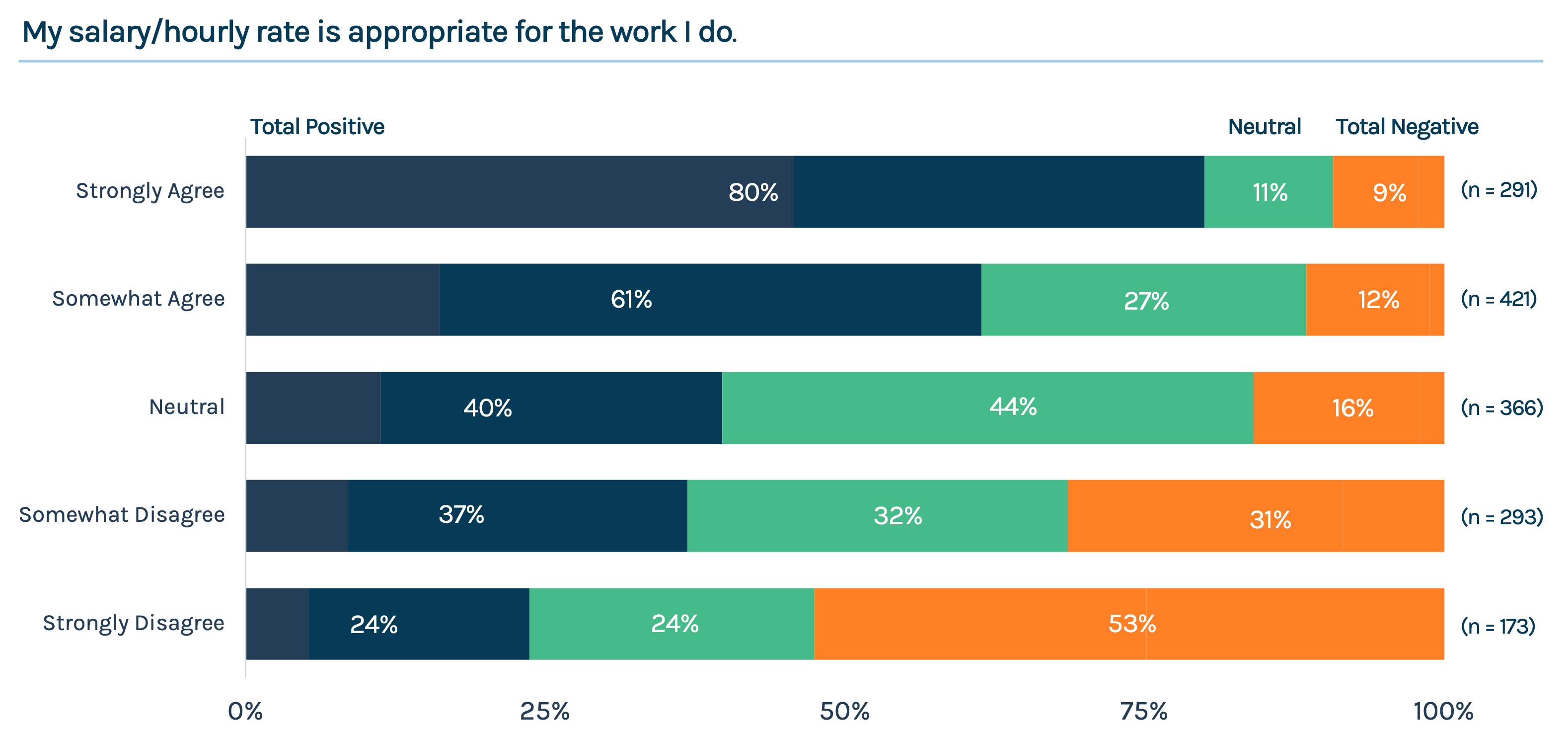
Barely half of nurses agree that their compensation is adequate for them to live comfortably, and only about one in four think their pay matches their work. It is this question – level of agreement about whether pay is appropriate for the work – that is used throughout this report to distinguish between nurses who are satisfied and dissatisfied with their compensation. Only a quarter of nurses are very satisfied with their job, with half saying they are very likely to stay in the field of nursing.
43
AGREE “MY SALARY/HOURLY RATE IS APPROPRIATE FOR THE WORK I DO.”
As a practicing healthcare worker, how satisfied are you with your job?
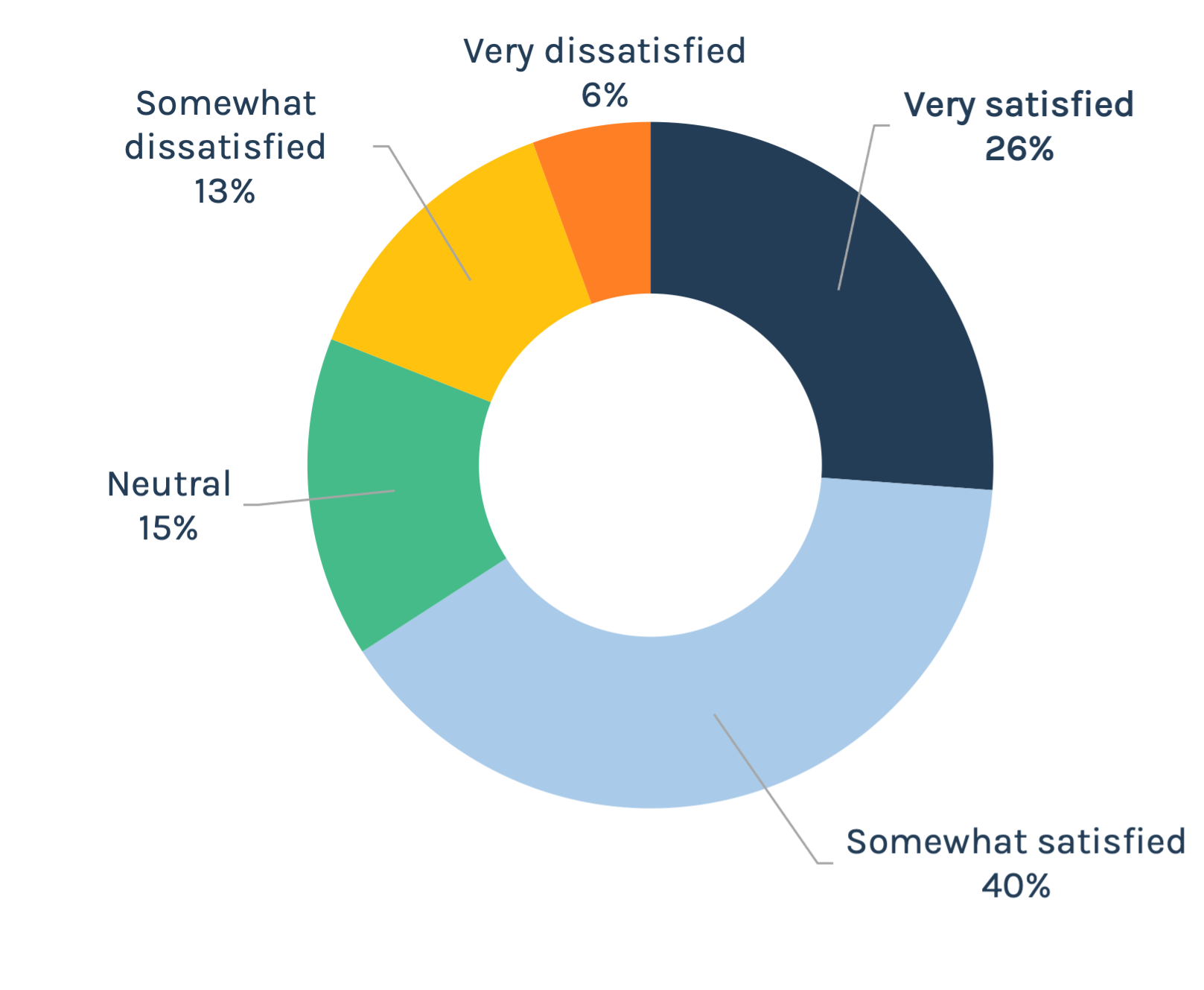
As a practicing healthcare worker, how satisfied are you with your job?
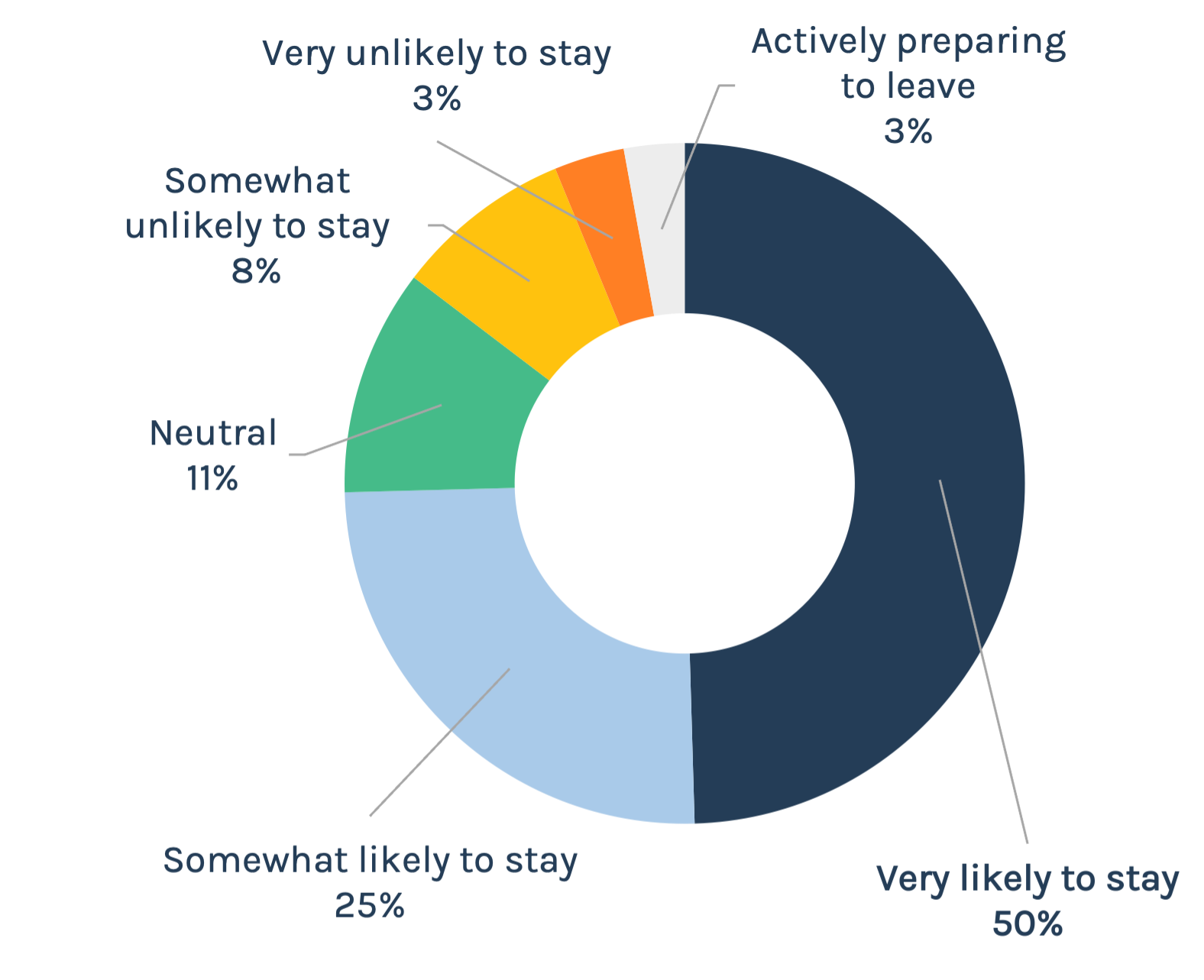
Finding 2: Trust is highest at the ground level
Nurses have greater trust in relationships with people they interact with on a regular basis, like colleagues and managers. Additionally, nurses view team dynamics more favorably than they do connection with and support by leadership and the organization. Fewer than half of nurses think their organization is effective at cascading information from administration to management and then on to team leads and staff. Though not tested here, deficient cascading may contribute to weaker connections between nurses and administration, lowering trust. Face-to-face conversations are considered the best way to help improve the cascading of information – team huddles, quick calls and the like.
Train for Trust
The maxim “People don’t leave their employers they leave their managers” is worth remembering here. The trust people have in their managers is something to be used, guarded and reinforced. There’s little correlation between being an outstanding technical expert – i.e., a great nurse – and being a great leader. Leaders need training to both manage well and build trust among their teams and also serve as an effective link between administration and front-line staff. Without that training, organizations risk weaker links between managers and staff, leading to costly turnover and lower morale.
Who is your most trusted source of information within your employer organization?
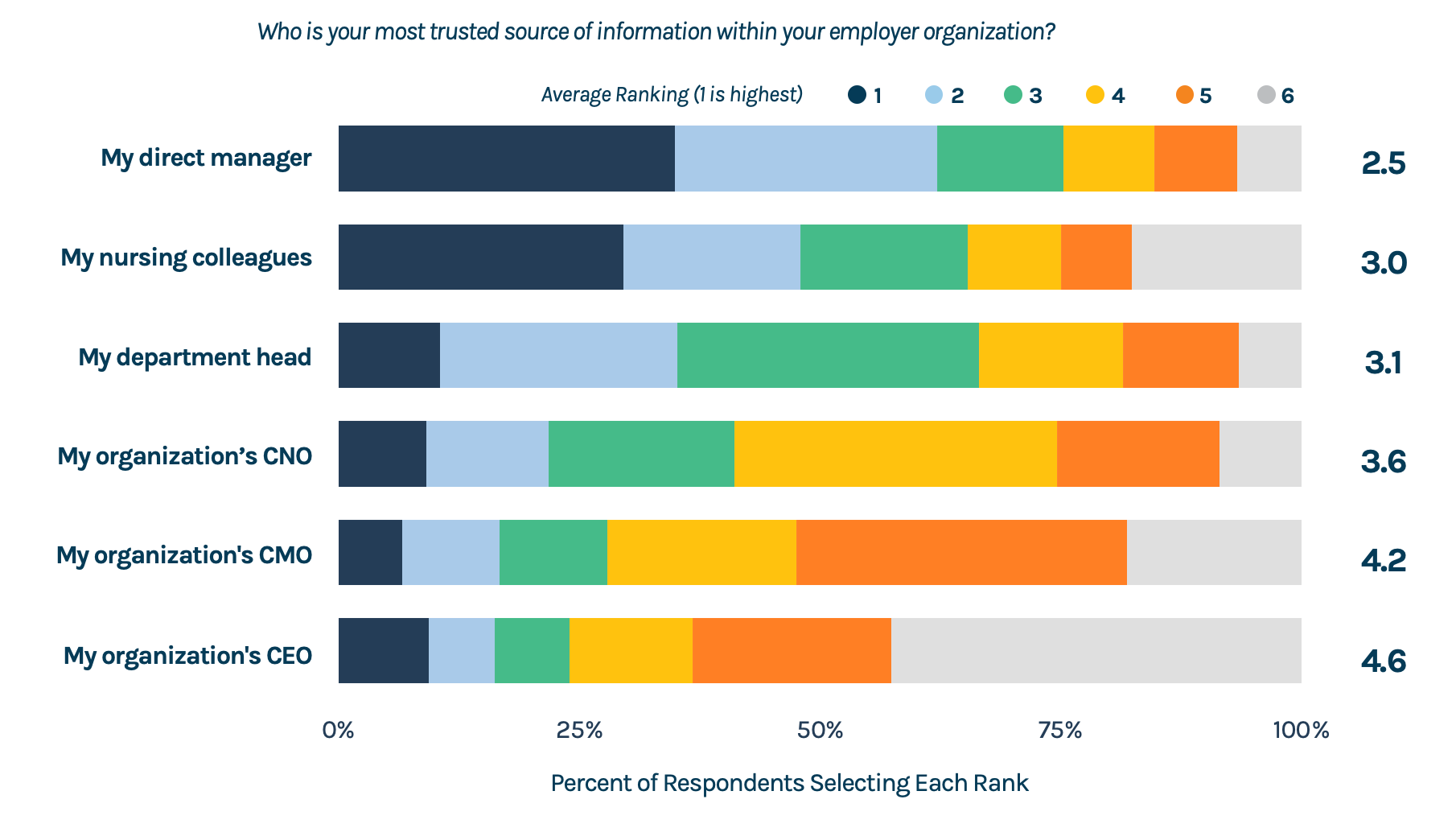
66
AGREE “TEAM DYNAMICS IN MY UNIT/AREA ARE POSITIVE.”
45
AGREE “MY ORGANIZATION HAS MY BACK.”
Finding 3: Engagement tactics are not one-size-fits-all
Nurses who feel they’re paid appropriately are more likely to appreciate non-financial offerings than nurses who feel their compensation is lacking. Nearly half of nurses said that increased staffing would be a helpful substitute for higher pay, with more than one in four saying that additional PTO would help. Among nurses who are dissatisfied with their pay, those numbers rose to more than half and nearly half, respectively. At the same time, nurses satisfied with their pay were more than twice as likely to feel more valued by global recognition events like Hospital Week, whereas nurses dissatisfied with pay were nearly twice as likely to consider Hospital Week tone deaf.
If your organization is unable to offer raises, or only able to offer small raises, would any of the following help make up for the situation? (Select up to three.)
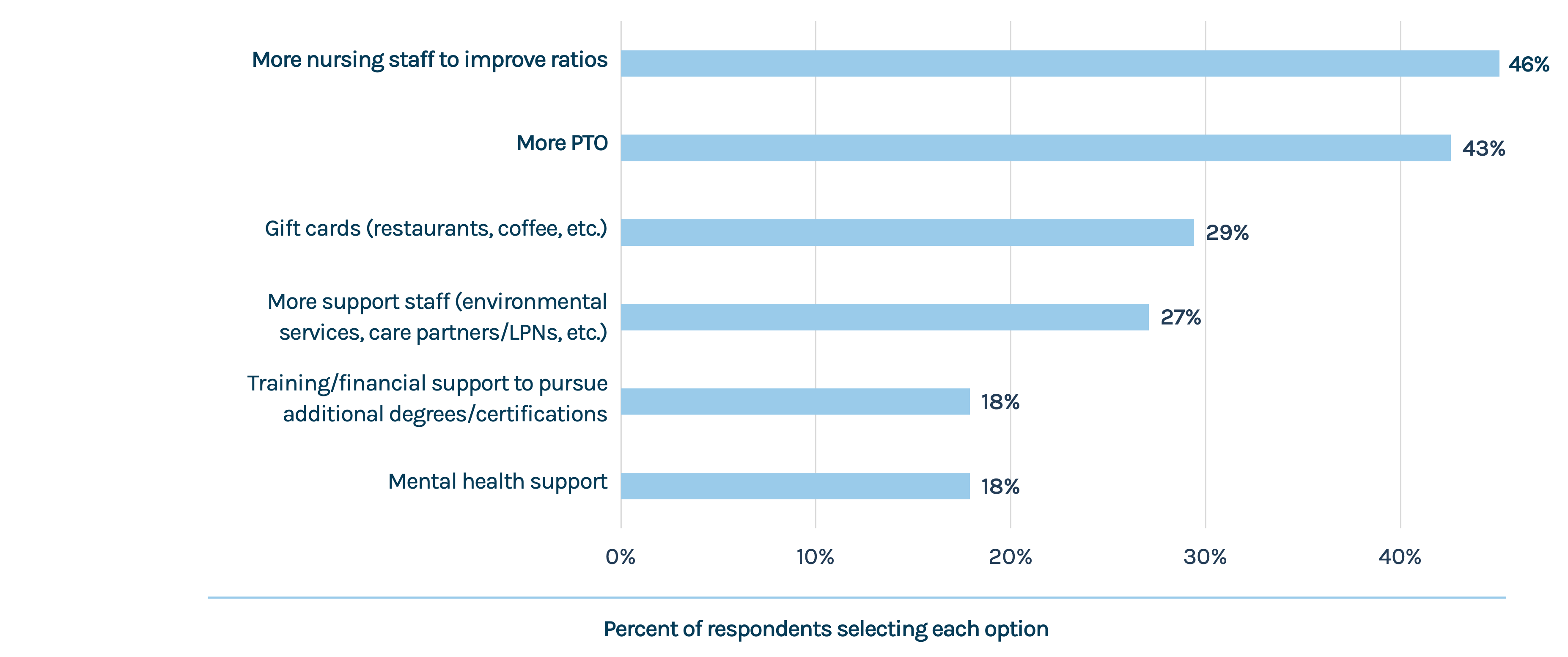
Which of the following most closely resembles your feelings about your employer’s approach to this year’s Hospital/Nurse/Employee Appreciation Week and similar events?
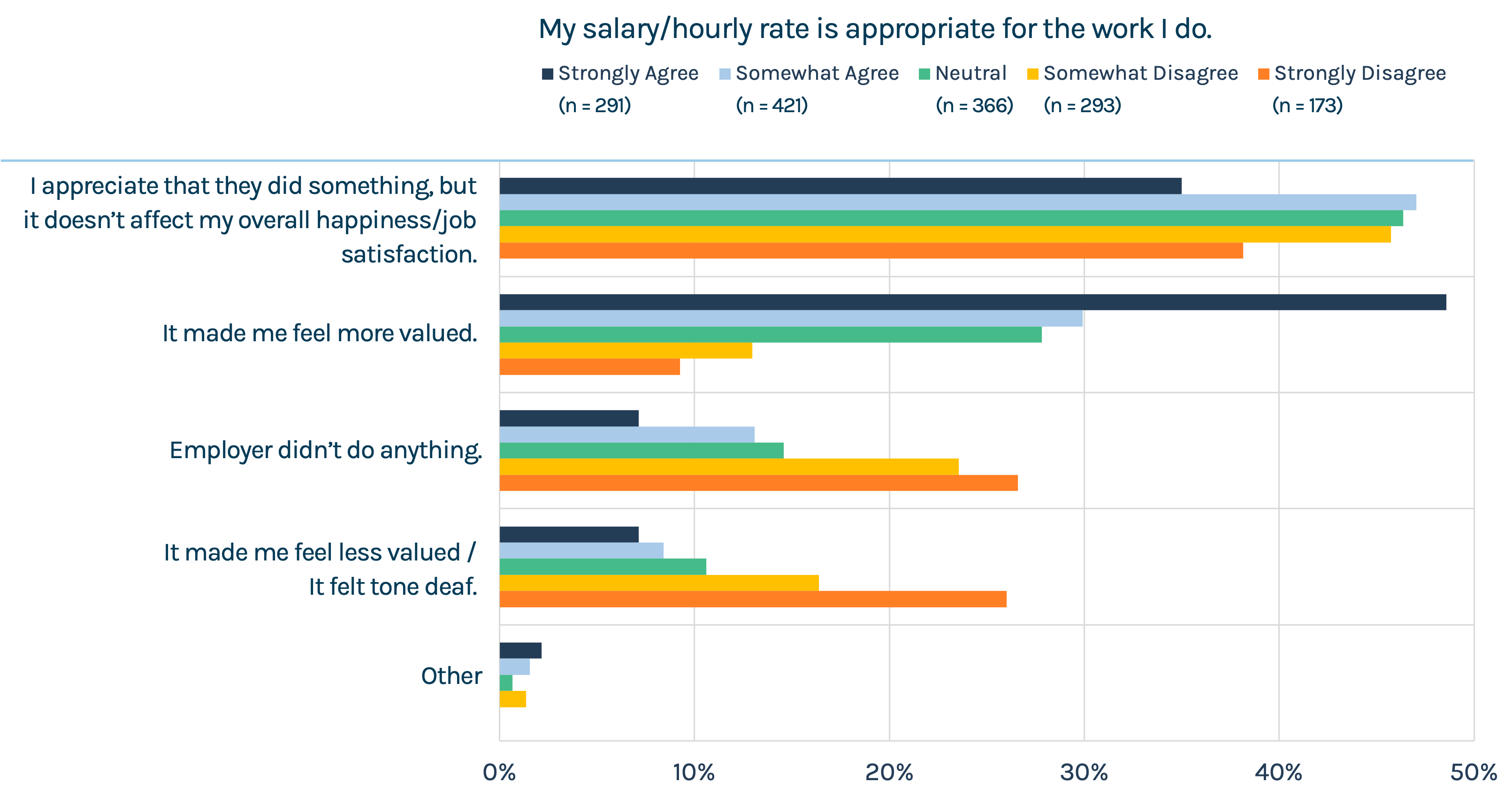
Finding 4: Intent isn’t enough for unhappy nurses
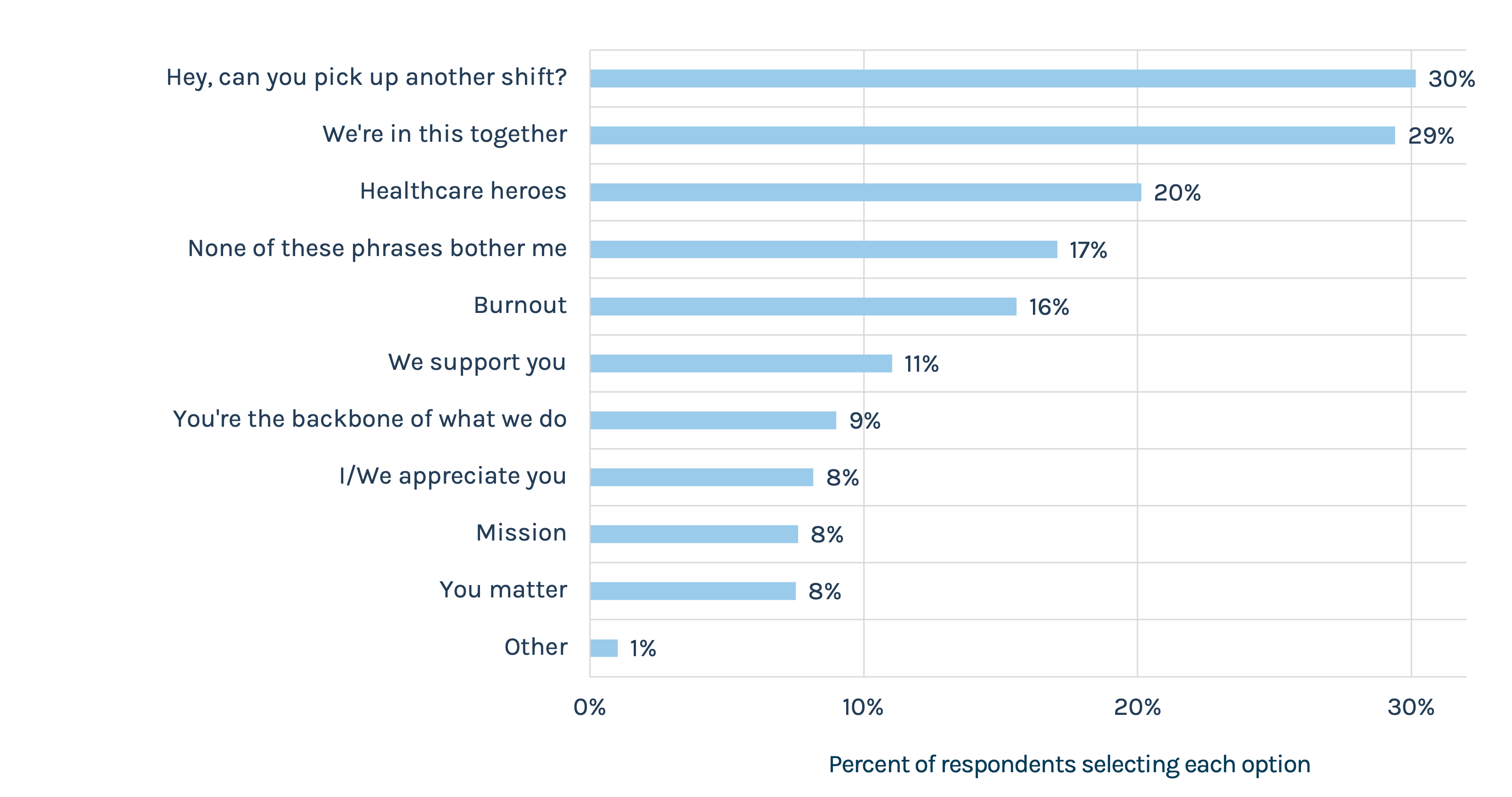
Those on units caring for patients day-in and day-out don’t want empathy layered with requests to do more. Or kitschy tokens of appreciation. Saying “We’re in this together” sounds hollow when you’re asking nurses to work more. Three in 10 nurses selected “We’re in this together” as a phrase they never wanted to hear again. In open text responses, nurses pointed out that pizza parties, pens and generic messages offered by leadership teams come across as tone deaf. Snacks and trinkets don’t match the message of “We appreciate you” and “We’re in this together” when what nurses are looking for are higher pay and more staffing. The instinct is to do something and that’s better than doing nothing at all. But that instinct, that assumption, can be problematic when nice gestures actually make things worse in the right (or wrong) context. It’s like medicine – apply carefully and in the right context, but more isn’t necessarily better.
What is the word/phrase/idea that you never want to hear again? (Select up to two.)
”They gave us inspirational rocks that were painted for Nurses Week. I am trying to make ends meet and pay bills. I want more money, not an inspirational rock and candy.
Compensation vs. Recognition
Along with results mentioned in Finding 3, these results demonstrate an important distinction: Compensation and recognition are viewed separately by employees and should be kept as such by leaders. Tactics to recognize nurses for their efforts can’t be used as substitutes for compensation. A pizza party or gift card or handwritten note is a valuable way to show nurses that their work is seen and appreciated. It’s not about the gift card, but what the gift card represents. For a nurse who feels appropriately compensated, it is more likely to be seen as recognition. For one who feels underpaid, it is more likely to be seen as a cheap attempt to make up the difference – to be seen as compensation.
Finding 5: Present, engaged and authentic leadership can help
If knick-knacks are counterproductive, deep engagement resonates. The nurses said thoughtful executive rounding coupled with clear communication, active listening and follow-up plans are bright spots that increase nurse satisfaction. There is, however, a connection between satisfaction with pay and executive rounding. Eight in 10 nurses who feel they are paid appropriately think that executive rounding has a positive effect on nurse satisfaction, with nearly nine in 10 saying it has positive effects on care team unity and effectiveness. It’s conceivable that there is a correlation between nurses feeling fairly compensated and higher levels of trust. Conversely, those who feel underpaid may be less trusting of leaders, even perceiving them as disingenuous.
What kind of effect do you believe executive rounding has on job satisfaction for nurses?
”They are making more frequent rounds now and trying to more actively listen. The new CEO has re-energized us.
Executive Visibility
Even though the relationship between manager and nurse is the most impactful, other relationships are also important. Building trust between nurses and the CNO, CMO or CEO is not mutually exclusive with promoting ground-level relationships. Good, well-trained managers will create a virtuous cycle of trust within their teams. As that flywheel turns, it creates room for organizations to find ways to make executives more accessible and build those vertical relationships. That makes the cascading of information more effective, helps nurses buy into the organization’s broader vision, and provides a stronger foundation for managers as they lead their teams.
Implications and Opportunities
These findings confirm what healthcare communications leaders’ instincts and experiences have been telling them for the past couple of years. A notable percentage of nurses are concerned about pay, and that dissatisfaction correlates with more negative feelings about a range of other work-related topics. But those feelings are not universal. It is there, in heterogeneity, that both risk and opportunity lie for healthcare leaders.
What this survey shows is that there is significant nuance in what nurses need today. Pay is not the only thing that nurses care about, and alternatives to raises or increased staffing are not one-size-fits-all. Therefore, relying on old tactics of global engagement risks alienating nurses needing something different. This is seen in the stark divide in perception about Hospital Week and executive rounding between nurses who feel appropriately compensated and those who don’t.
The conversation nurses are having encompasses lifestyle, stress, balance and a desire to work in an organization where words of appreciation are matched by actions that show appreciation and respect. Executives must ensure that they are hearing those concerns and not talking past caregivers. Doing so only leads to broken trust and further disgruntlement, making further actions ring even more hollow.
Helping align the conversation is a core imperative for communications leaders. Specifically, they can guide their organizations towards a nuanced approach to engagement and refine processes that build relationships top to bottom. That, in turn, leads to a better cascade of information and greater connection with shared goals. And, critically, greater satisfaction – even in the absence of increasing nursing staff or massive pay raises.
To get started, here are a few opportunities to bolster and engage the nursing workforce.
Bring Clarity to the Conversation
In the current climate, the things we’ve done in the past don’t resonate in the desired way. As nurses tune out broad messages and gestures, communicators need to be intentional about clarity, listening and meeting nurses where they are.
Invest in Training Your Frontline Managers
With direct relationships between nurses and managers the strongest within the nursing hierarchy, leaders at all levels need to be trained as communicators and equipped to build those relationships and cascade information on behalf of the organization.
Stop Doing What’s Tone Deaf
Some tactics for boosting nurse satisfaction come across as missing the mark, especially for nurses who feel they aren’t paid appropriately. Though well-intentioned, these may do more harm than good. Consider changing your approach, offering different options and providing clear communications about what is happening and why.
To help your organization chart its path forward, we invite you to fill out the form for full survey results.
Subscribe to Jarrard Insights & News
"*" indicates required fields




